3 Didactic Day 3
ALCOHOLISM
Learning Objectives
- Screen for alcoholism
- Use motivational interviewing with patients with alcohol misuse
Required Video: Alcoholism
Required Reading: Screening Tools for Unhealthy Alcohol Use
Required Reading: Pharmacotherapy for Adults with Alcohol Use Disorder
Resource: Alcoholics Anonymous
Resource: SmartRecovery
Video: Alcoholism
Poul LaPlante MD 3/14/17
Underdiagnosis
- In primary care and hospitalized patients ETOH problem only diagnosed in about 40% of those suffering from it 1
Reasons for Underdiagnosis
- Lack of organized approach to diagnosis and treatment
- Denial prominent in alcohol problems, especially minimizing use
- Potential for conflict in confrontation with patients
- Feeling that this is not a medical problem 2
Diagnostic Tools (over 200)
- CAGE (1964): 4 questions; simple; best for severe disease
- MAST and others: 10-30 questions; sensitive; time-consuming
- AUDIT: current gold standard; 10 questions; Sensitive; somewhat time-consuming
Drinkers When Quitting Complain Most
- Do you drink? If no, why not (US 60% adults drink alcohol)
- When was your last drink? (default 1-2 days )
- Ever cut down or quit? Normal drinkers don’t have to cut down or quit except in pregnancy or weight loss. Very high sensitivity for alcohol use disorder
- Has anyone complained about your drinking? Highest sensitivity
- Largest amount consumed in 1 sitting? Past year? + is ≥ 7 drinks for men, 5 for women
Associated Points of History
- Legal: 2 DUI arrests has extremely high sensitivity for presence of an alcohol use disorder
- Family History: 60% of alcoholics in detox have 1st degree relative with the disease
- Blackouts, injuries, morning drinking, drinking alone, unable to stop, previous treatment or AA, drink every day, drinking when unplanned or will affect responsibility, other drug use, tobacco use
Communicating Diagnosis
- Refer to “problems with alcohol” or “alcohol use disorder” rather than alcoholism
- Remain factual and neutral
- State why you are concerned (factual evidence)
- Talk about denial
- Outline natural history of alcohol misuse
Helping Patient Accept Diagnosis
- Get patients definition of alcohol problem
- Offer alternatives for definition
- “If drinking causes problems and you keep drinking, you have a drinking problem”
- “Inconsistent Inability to control Intake”
Treatment
- Evaluate for need of withdrawal management
- Suggest abstinence, if patient insists on moderating drinking
- Alcohol challenge test
- Suggest “Open” AA meeting; frame it in terms of learning more
- Deal with objections which may arise such as: God, bad with groups, will power, shy, afraid they will see people they know
Other Resources
- Smart recovery: good program, not many meetings
- Rational Recovery: online only
- LICSW, psychiatrists, and others who have experience with addictions
Follow Up
- Inquire as to drinking status each visit; If someone is not receptive to talking about it today, they may be more open in the future.
- Avoid Benzodiazepines. If patient is unable to stay sober and is depressed, consider SSRI
- Adjunctive medications such as naltrexone, acamprosate, disulfiram of limited utility
References
- Moore, Richard. “Underdiagnosis” Journal of Medical Education (1987) 46-52
- Clark, William. “Primary Care Physician and the Patient with Alcoholism” American Journal of Medicine (1981) 275-286
Visnuth Keo: Smoking Cessation
Case
Visnuth Keo is a 35 yo Cambodian-American male who works as a nurse in a nearby nursing home. His work requires that he be screened for tuberculosis annually. He comes today to get that done.
The medical assistant in the office identifies Visnuth as a current smoker on the Electronic Health Record (EHR).
Questions to Consider
- What do you say to the patient about his current smoking status?
- Using the Prochaska Model of Lifestyle Modification, what stage is Mr. Keo in?
- How do you bring Mr. Keo from his current stage to the next stage?
- How do you quantify how much Mr. Keo is addicted to nicotine?
Learning Objectives
By the end of the session, the active participant will be able to:
- Explain how office systems can help a physician more efficiently and effectively screen for cigarette use and counsel on smoking cessation.
- Assess what stage a patient is in using the Prochaska Model of Lifestyle Modification and be able to use this model to counsel patients on other subjects.
- Describe the multiple modalities available to assist a patient in quitting smoking.
Required Reading: Promoting Smoking Cessation
Handout: Smoking Cessation Therapy
Resource: Smoking Cessation Worksheet/Contract
| TIMES OF THE DAY I AM MOST TEMPTED TO SMOKE | WHAT I CAN DO INSTEAD OF SMOKING DURING THOSE TIME |
| 1 | 1 |
| 2 | 2 |
| 3 | 3 |
| 4 | 4 |
| 5 | 5 |
| Quit Date: | Today’s Date: |
| Signature: | Provider’s Signature |
Example of how a patient completed this worksheet:
| Must Have Cigs | Things I Can Do Other Than Smoke!! |
| 1. First thing in the morning | a. Sit ups
b. Read c. Have sex |
| 2. Riding into work | a. Think about the kids
b. Plan my work better c. Picture my life without cigs d. Write a song |
| 3. Breaks at work | a. Go outside |
| 4. After dinner | a. Play with the kids
b. Ride my bike c. Do yard work d. Play guitar |
| 5. At night after kids go to bed | a. Read
b. Play guitar c. Work out d. Have sex |
Health Systems
Learning Objectives
- Define the quadruple aim
- Describe factors that contribute to the high cost of US healthcare
Required Reading: From Triple to Quadruple Aim
Required Reading: The Developing Vision of Primary Care
Required Reading: Overkill
Optional Reading: The 10 Building Blocks of High Functioning Primary Care
Optional Reading: 100 Million Healthier Lives Concept Paper
Motivational Interviewing
Motivational Interviewing
“Motivational interviewing is a directive, patient-centered counseling style for eliciting behavior change by helping patients explore and resolve ambivalence” – Stephen Rollnick & William R. Miller
Learning Objectives
- To describe the usefulness of motivational interviewing in changing patient behavior
- To identify the principles of motivational interviewing
- To practice specific techniques to facilitate effective motivational interviewing
- To implement motivational interviewing into routine patient interviews
Think of a time in your life when someone inspired or motivated you to make a big change – how did they do that?
To begin, assess patient’s readiness to change: Pre-contemplative/Contemplative/Preparation/Action/Maintenance/Relapse
4 Principles of Motivational Interviewing – “REAL”
- R – Righting reflex
Doctors are trained to make things right, and do this with our “righting reflex”. We want to tell patients what to do in order to fix them. Techniques often used are: suggesting, advising, persuading and giving speeches. These techniques usually shut patients down.
Avoid the righting reflex. Avoid arguing, ordering, directing, commanding, warning, threatening, telling patients what they should do, advising, suggesting solutions, persuading with logic, disagreeing, judging, criticizing, probing, interrogating.
In order to help patients, try to listen and engage them. Dance-don’t wrestle- with resistance (Rolling with resistance example: sounds like quitting smoking will never happen for you, I didn’t say never). Allow patients to explore barriers in a nonjudgmental, supportive manner to help them to change.
- E – Empathy
Express empathy. This helps to build trust and collaboration, legitimizes patient’s struggle, and communicates respect.
Techniques include:
- Ask for permission: “Would you be willing to discuss your smoking?”
- Reflective listening: “What I hear you saying is that drinking helps you manage your stress”
- Open ended questions: “What do you think it would be like to take your insulin?
- A – Ambivalence
Explore ambivalence and uncover discrepancy through active listening. This helps patients figure out what they are doing vs. what they want to be doing (uncover discrepancies between the patient’s behavior and values).
Techniques include:
- Open ended questions about specific concerns: “What concerns you most about your smoking?”
- Facilitating recall about times before the behavior was a problem: “What was it like for you before your drinking started affecting your work?”
- Facilitating patient imagination of future both with/without behavior: “What do you think your life will be like in five years if you don’t change the way you are eating?”
- Connecting patient’s values with behaviors/Explore ambivalence: “What do you like about smoking? What do you not like about smoking?”
- Use scaling questions: “How important is it for you to do this on a scale of 1-10- 10 being most important. Why did you pick a 6 instead of a 3? What would it take for you to be a 9?”
- L- Listen in order to Understand and Empower
Listen to what your patients are really saying, listen to the changes they are willing to make, and support their self-efficacy Use active listening techniques, open ended questions, and reflect and clarify what you hear.
- Support your patient’s strengths, successes and provide encouragement.
- Communicate to patients that they are in control of decisions, and that you are there to provide support and guidance.
- Help patients in make self-generated action plans. When the patient “owns” the plan they’re more likely to execute it.
- Facilitate follow-up on the plan.
Analogy: Car with emergency brake half on…Grind forward as fast as you can and wonder why it feels so hard or, recognize that the patient is the driver and motivate him/her to turn the emergency brake off.
Evidence to support Motivational Interviewing:
A meta-analysis done by Vasilaki in 2006 reviewed 9 studies comparing brief motivational interviewing with other interventions for treatment of excessive alcohol use and found that it was more effective than the traditional approaches.
Motivational interviewing was also found to be effective in studies looking at behavioral interventions in teens with type 1 diabetes (Channon et al 2007) and obese women with type 2 diabetes (West et al 2007). In a study of a behavioral weight loss modification program, adding motivational interviewing led to increased weight loss, improved physical fitness, and improved dietary intake as compared to the group without motivational interviewing (Carels et al 2007).
References:
Using motivational interviewing as a supplement to obesity treatment: a stepped-care approach. Health psychology: official journal of the Division of Health Psychology, American Psychological Association 26(3):369-74
Motivational Interviewing In Teenagers with Diabetes
Motivational Interviewing Course: Arizona Center for Integrative Medicine; Integrative Medicine in Residency 2013
Behavioural and Cognitive Psychotherapy
Motivational interviewing improves weight loss in women with type 2 diabetes
Created by Wayne Altman, MD, FAAFP
Nutrition/Obesity
Required Reading: Diets for Health: Goals and Guidelines
Optional:
Handout: Nutrition Truth
Handout: Altman Rule
Case
Terry McHale is a 58 year old patient coming in for a follow up visit. Terry was seen 2 weeks ago for a physical by
your partner who is now on maternity leave. Terry is here today as instructed for lab results. The patient has a strong
family history for coronary artery disease: Terry’s father died of a heart attack and older brother had
quadruple bypass at 52.
Use this visit to review vitals / labs, gauge Terry’s stage of change, discuss with Terry your concerns about their health, elicit their values, and engage Terry in change-talk aligned with those values.
BP 140/90 (2 weeks ago, BP was 138/85)
Pulse 90
Weight 222
Height 5’11”
BMI 31
Total Cholesterol 260; LDL 175; HDL 45; Triglycerides 200
Fasting glucose 88
Learning Objectives
- Describe evidence-based nutrition plans (diets for health)
- Counsel a patient on nutrition
- Name the benefits of healthy eating with respect to cardiac and chronic disease risk factors
Christine McHale: Pregnancy Options
Case
Christine McHale is a 24 year old female. It’s been 8 months since you last saw her in the office and she comes in today because her period is 5 days late. The nurse has done a urine pregnancy test which is positive, but she hasn’t given Christine the results. Christine has come to the office with her boyfriend, Marc, and they are waiting in the exam room together.
Questions to Consider
- How do you give the news of the positive pregnancy test?
- What are Christine’s options for this pregnancy?
- Is emergency contraception an option?
- What are the key facts women need to know when deciding about adoption, medical or surgical abortion?
- What are the reasons a woman may choose a medical versus surgical abortion or vice versa?
- What counseling techniques can you use to help her through the process of making a decision?
- If a provider is ethically opposed to abortion what are his/her obligations when caring for a patient who presents for options counseling or abortion care?
- What question(s) would you find hardest to answer or what clinical scenario(s) do you fear most when it comes to options counseling or abortion care? Write them down on your index card.
Learning Objectives
Learners will be able to give the news of a positive pregnancy test and counsel a patient with an unintended pregnancy about the basics of her pregnancy options (parenting, abortion and adoption) in a nonjudgmental, non-directional, and patient-centered manner.
Learners will be able to provide evidence-based answers to patients’ frequently asked questions about emergency contraception and early abortion options.
Required Reading: Fact Sheet on Induced Abortion in the United States
Required Reading: Emergency Contraception and Medication Abortion: What’s the Difference?
Required Reading: Comparison of Early Abortion Options – A Resource for Patients
Required Reading: BMJ Clinical Review: Abortion
Resources:
Pregnancy Options Info: A Workbook of Options including Abortion, Adoption, and Birth
Fact sheet for families from the Department of Health and Human Services: “Are you pregnant and thinking about adoption?”
Reproductive Health Access Project. Resources to help primary care physicians provide contraception and abortion care.
ACOG Committee Opinion: The Limits of Conscientious Refusal in Reproductive Medicine
ANSIRH Early Abortion Training Workbook
Sports Medicine Workshop
Learning Objectives
- Perform a knee and a shoulder exam
- Describe common pathologies of the large joints and their treatments
Required Reading: Patellofemoral Pain Syndrome
Required reading: Shoulder Pain
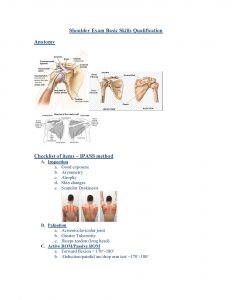
Technique to examine joint: “IPASS”
- Inspection
- Palpation
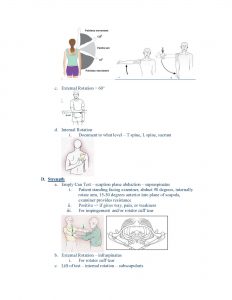
- Active Range of Motion
- Strength
- Special Tests